Phimosis
Phimosis is a constriction of the foreskin that, if left untreated, can produce symptoms such as pain during erection and urination.
WHAT IS the PHIMOSIS?
Phimosis is a foreskin narrowing. The foreskin covers and protects the glans, which is the penile end. The narrowing is most noticeable between the inner and outer leaflets of the foreskin. This prevents the foreskin from rubbing on the glans.
There are three levels of phimosis reported
- With mild phimosis, you can expose the entire glans. The narrowing is at the level of the penis's body, and the uncovering manoeuvre is difficult; you may experience pain or discomfort.
- Moderate phimosis allows for partial exposure of the urethral meatus, the urethra's external opening. Intimate hygiene is difficult.
- Severe phimosis: the meatus cannot be exposed. As a result, keeping clean is impossible, which can lead to both local infections and urinary tract infections.
What factors contribute to phimosis?
Phimosis is caused in 99% of cases by inflammation (balanoposthitis or xerotic balanitis obliterans) or trauma from clumsy manoeuvres. In most cases, the foreskin does not flow sufficiently to reveal the glans in early children.
As a result, foreskin narrowing is considered normal in the first years of life. It is present in 80% of newborns at six months, 10% of children at three years, and 1% of children at five years, after which the foreskin normally separates from the glans in 90% of cases.
As a result, it is proper to speak of phimosis only after this age.
In adults, phimosis is frequently caused by persistent inflammation, which occurs when the foreskin does not retract during urination. Urine in direct touch with the skin weakens the immune system and promotes persistent inflammation. This increases the likelihood of fungus and bacteria infecting the foreskin and glans.
What are the signs and symptoms of phimosis?
Phimosis in a pre-adolescent patient does not normally manifest itself. It can induce dysuria (difficulty urinating), pain during erections, and sexual intercourse problems in adolescence, especially in the most severe types.
Balanoposthitis, a fungal or bacterial infection that affects the glans and the foreskin that covers it, is the most common type of inflammation. Balanoposthitis is distinguished by localised redness, the presence of fluids, swelling, and irritation.
Paraphimosis, on the other hand, is caused by a forceful retraction of the foreskin and is a complication of phimosis. It can only be resolved with the doctor's prompt action.
After the age of five, the diagnosis is based on a meticulous review of the child's medical history and an equally thorough examination. The inability to retract the foreskin and discover the glans during the visit provides the diagnosis in the most severe cases. When retraction is possible, the disease is identified by examining the "hourglass" shape of the penis as the foreskin is slid over the glans and over the penis.
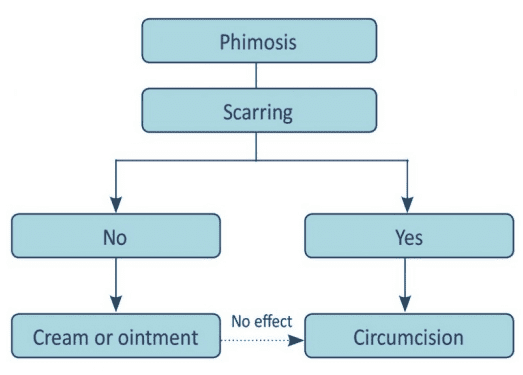
The most effective treatment for phimosis is betamethasone (0.05%) given topically twice a day for a month. When you apply a cream with cortisone in it, you can minimise inflammation in the skin of the foreskin and restore its normal flexibility.
It is critical to link betamethasone therapy with foreskin stretching: softly and safely glide the foreskin on the glans to dilate it. After receiving sufficient training from a doctor or health care provider, parents can undertake this manoeuvre.
If a month's worth of treatment does not completely fix the problem but is still effective, it should be continued for another month.
To keep relapses under control, the patient should be seen every 4-6 months after therapy. In cases of failure to heal phimosis (resistance to treatment or deterioration) or phimosis linked with recurring infections, surgical surgery is indicated.







