What is testosterone, and how does it affect the male body?
Testosterone is a steroid hormone found in both men and women. It is produced in large quantities in males throughout their lives by Leydig cells situated inside the testicles. In women's case, testosterone, produced in both the ovaries and the adrenal glands, is mainly converted into oestrogen by the aromatase enzyme.
Testosterone is primarily essential for the development of male body secondary sexual traits such as a beard and overall villosity, muscle bulk, and a deep voice.
It also influences erection, sperm production, genital growth, and individual desire.
Finally, having the proper testosterone level aids in regulating mood and thinking processes, as well as synthesising red blood cells in the blood.
What are the typical testosterone levels?
The testosterone concentration in the blood fluctuates with age, peaking during early adulthood and significantly decreasing from 40-50 years, leading to andropause in the following decades.
According to Mayo Clinic laboratory data, a man's typical testosterone levels should be in the following ranges:
- From 0 to 5 months, the range was 75-400 ng/dL.
- From 6 months to 9 years, the range is 7 to 20 ng/dL.
- The range for youngsters aged 10 to 11 is 7 to 130 ng/dL.
- 7-800 ng/dL between the ages of 12 and 13
- 7 - 1,200 ng/dL at 14 years old
- 100 - 1,200 ng/dL between the ages of 15 and 16
- 300 - 1,200 ng/dL between the ages of 17 and 18
- After the age of 19, 240 - 950 ng/dL

If testosterone levels are aberrant within this range, two scenarios may occur.
The first scenario
The second scenario
Men's low testosterone causes and symptoms
Except for substantial external conditions that can impair testosterone synthesis, a low amount of this hormone within a male man is frequently associated with various thyroid, genital apparatus, or cardio-circulatory system illnesses. Substance abuse, alcoholism, and depressive disorders can also suppress testosterone levels.
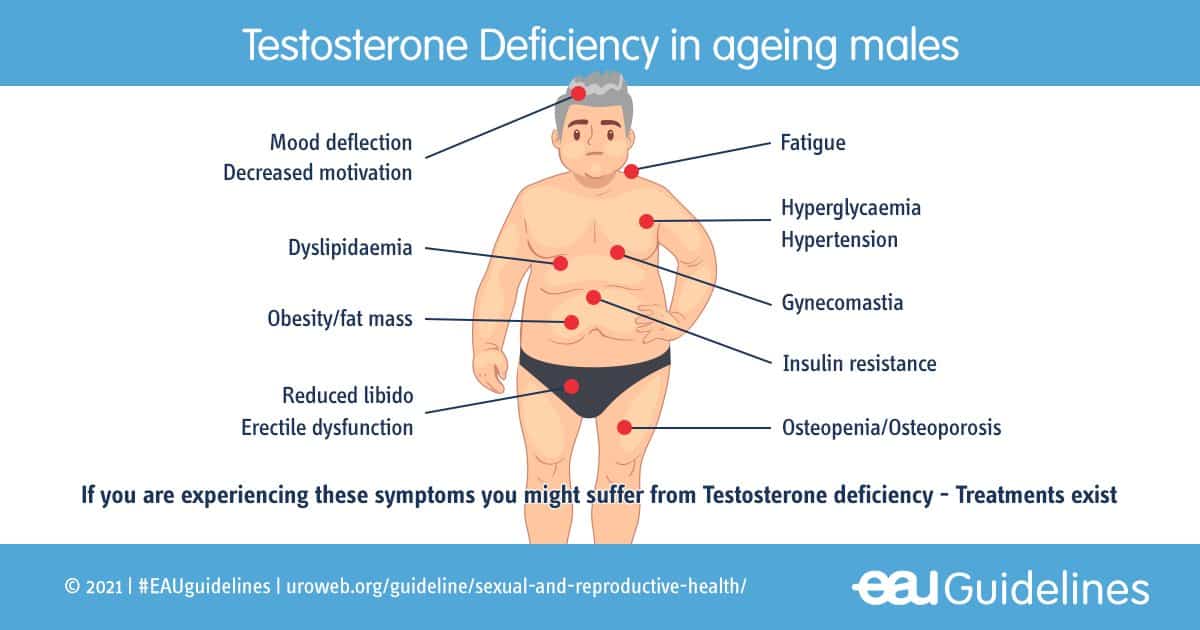
Given the nature of the components of the body that this hormone governs, the symptoms of testosterone insufficiency in males primarily affect the reproductive and sexual spheres and extend to the overall psychological state. These warning signs include
- Erection problems
- Lowered libido
- Infertility in men
- Asthenia, tiredness, and depression
- Loss of hair
- Loss of muscle mass and bone density
- Puberty is delayed, and genital development begins at a young age.
As previously stated, puberty and adolescence are when testosterone production peaks before plateauing in maturity. Low testosterone levels in young people can be noticed in their slower sexual development and increased secondary sexual features.
However, anatomically, the consequences of a low testosterone level at a young age include a lack of or limited development of the genital organs.
Once a person enters maturity, testosterone levels continue to fall by 1% per year. This continues until the so-called andropause, a word based on female menopause, indicates that a man's reproductive capacities have naturally run out rather than something wrong.
As a result, a steady drop in testosterone levels in the blood should be seen as a normal component of the ageing process and should not be regarded as cause for alarm. Assume, however, that testosterone levels are low and are connected with the symptoms listed above. The general practitioner will then be able to determine how to treat them to return them to stable levels.
Monitoring testosterone levels: the essential tests
Blood tests are required to monitor testosterone levels, which allow for the measurement of two useful statistics in determining any disparities in the presence of the hormone:
Blood testosterone is the portion of testosterone associated with sex hormone-binding globulin (SBHG), a protein that transports sex hormones throughout the body. The free testosterone test will tell you how much of this hormone is in your blood overall.
The free portion of testosterone circulating in the body is represented by free blood testosterone. The free testosterone test assesses the physiologically active hormone.
These tests can be scheduled swiftly at the linked facilities, even without a prescription. Still, if you suspect your testosterone levels are low, consult your doctor first.
If a low testosterone level is discovered together with other discrepancies in blood test results, it can be a symptom of other, more severe disorders, such as:
- Hypogonadism (reduced or interrupted production of the hormone by the sex glands)
- Inadequacy of the testicles
- Diabetes and nephropathy are two chronic diseases.
- Severe obesity
- Malignancy of the testicles
As a result, if testosterone levels are significantly lower than average and one or more of the symptoms listed in the corresponding paragraph are present, the patient's general practitioner or competent endocrinologist may recommend a pharmacological treatment to replenish the amount of testosterone present in the body.
Treatments and treatments for increasing testosterone levels

Thus, testosterone therapy is a point of arrival whose purpose is to counteract the effects of hypogonadism; it is not to be interpreted as a way of reversing the natural consequences of time on the male body, nor as a substitute for a correct helpful lifestyle for maintaining psychophysical balance.
In the absence of additional comorbidities, there are various strategies to maintain testosterone levels under control.
The first step in maintaining regular testosterone production is to eat a healthy and balanced diet; limiting your intake of foods with a high glycemic index, as well as the general health benefits, assist prevent the transition of testosterone to oestrogen via the aromatase enzyme. It is a physical activity that can, directly and indirectly, promote testosterone production.
Magnesium-rich foods, such as dried fruit, some types of fish, legumes, and cow's milk, also increase testosterone production. Even vitamin D, whose receptors are present in the reproductive system tissues where testosterone is produced, aids in increasing its levels; as a result, it is recommended to incorporate foods such as fatty fish and egg yolk into your diet, as well as to expose yourself to the sun with the necessary protection regularly.
Finally, the antioxidants found in fruits and vegetables, essential micronutrients for maintaining cellular balance, should not be overlooked.
Drug therapy is never used in the case of people with normal hormone levels, as outlined by the US Society of Endocrinology standards and followed by the international medical community.
Several methods of medication therapy can be used to give testosterone:
Injection: this is the most convenient procedure, but it subjects the patient to cyclic injections and fluctuating testosterone levels.Oral therapy: allows for more flexibility and autonomy in dosage, but it is susceptible to the influence of the liver and kidneys on testosterone hormone metabolism. This topical formulation helps you keep a consistent testosterone level in your body, but it has a high risk of discomfort.
Topical gel: The most novel method of administering testosterone is to apply the gel to the upper part of the arms once a day. The gel absorbs rapidly and does not pose any practical issues.
Before starting hormone therapy, the attending physician must rule out contraindications and assess the relationship between the benefits and adverse effects. The most common side effects are increased prostate volume, thrombi formation due to increased blood haemoglobin and haematocrit levels, sleep apnea, and water retention.







